Why innovation — not just effort — separates the best EMS billing partner from the rest.
When an EMS provider chooses an EMS billing company, the conversation often centers on collection rates, staffing, and customer service. Those things matter. But there is a deeper question that rarely gets asked: Does your billing partner actually own and protect its technology, or is it running the same generic processes everyone else uses?
At EMERGICON, the answer is clear. We have invested nearly two decades in building proprietary systems that are now protected by issued patents and pending patent applications — a portfolio that covers virtually every stage of the EMS billing lifecycle. For EMS leaders evaluating billing partners, understanding what those patents represent is understanding why our outcomes consistently outperform the industry.
Who We Are: Two Decades of Texas EMS Expertise
Founded in 2006 and headquartered in Dallas, EMERGICON is the largest EMS billing and collections provider in Texas. We serve more than 200 Texas EMS providers, generating annual cash collections of more than $200 million on their behalf. Our sister company, EMERGIFIRE, extends that expertise to fire and hazmat service providers and now serves over 70 Texas agencies.
We are not a national company that happens to serve Texas. We are a Texas company — built specifically for Texas providers, staffed by Texans, and operating exclusively within this state’s regulatory and payer environment. Every rule, every payer quirk, every Medicaid nuance we understand was learned here, applied here, and refined here for 20 years.
That specialization is the foundation. The technology built on top of it is what makes our results defensible, consistent, and scalable.
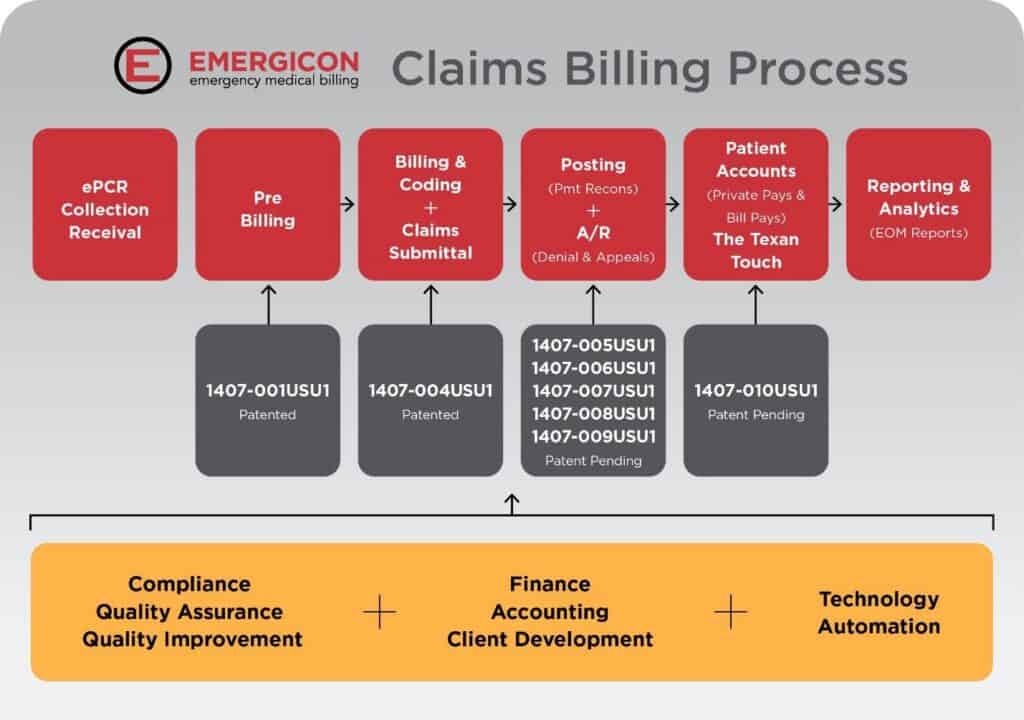
A Claims Process Engineered — and Protected — From Start to Finish
Most billing companies manage claims. EMERGICON has engineered a proprietary, end-to-end claims lifecycle and protected each stage of it through the U.S. Patent and Trademark Office. Here is what that looks like in practice.
Stage 1: ePCR Collection and Pre-Billing
Patent No. 1407-001USU1 (Issued) | Patent No. 1407-003USU1 (Issued)
The moment a transport record is received, our process begins. EMERGICON initiates pre-billing immediately upon receipt of the ePCR, requesting face sheets, payer information, demographics, and any missing data from the receiving facility via the fastest available channel.
What sets our pre-billing process apart is the time-bound escalation workflow protected by our issued patents. If data is not received within 24 hours, an EMERGICON team member contacts the facility directly. If it is not received within 48 hours, we resend and follow up repeatedly until all claim-critical elements are secured. No data gap goes unaddressed, and no claim moves forward incompletely.
This early discipline is where collections are won or lost. Getting it right before a claim is submitted prevents the denials, delays, and write-offs that plague less rigorous operations.
Stage 2: Billing, Coding, and Claims Submittal
Patent No. 1407-004USU1 (Issued)
Each transport is converted into a clean, compliant claim through a patented, standardized workflow that emphasizes accuracy, payer-specific requirements, and auditability. Our technology systematically estimates charges for the claim, and then every claim is reviewed by a human team member for completeness, coded, validated, and submitted electronically through our clearinghouse.
We submit electronically to all known and applicable payers: Medicare, Medicaid, commercial insurance, auto insurance, workers’ compensation, and attorney/third-party payers. Pre-submission claim audits check required fields, coding logic, and payer-specific submission rules before anything goes out the door.
We also want to be clear about something: we use humans, not computers, to read and code EMS charts. Technology supports our team — it does not replace the clinical and coding judgment required for accurate EMS billing.
Stage 3: Payment Posting, Reconciliation, and Accounts Receivable
Patent Applications 1407-005USU1, 1407-006USU1, 1407-007USU1, 1407-008USU1, 1407-009USU1 (Pending)
This is where many billing companies fall short — and where our technology creates the most measurable advantage.
Our payment posting process ensures that all payments — whether received electronically, through lockbox services, or via credit card — are accurately posted and reconciled. Our proprietary technology, described in our pending patent applications, analyzes financial transaction data across multiple payment formats, normalizes it, and identifies discrepancies requiring review. Posting errors are caught. Remittance data is reconciled. Financial reporting stays clean.
On the accounts receivable side, our pending patent applications describe predictive classification models that analyze historical claim outcomes, payer behavior, and account attributes to prioritize which claims require immediate attention. Our AR specialists are not working from aging reports alone — they are guided by a system that tells them which accounts are most likely to benefit from intervention right now. That focus accelerates reimbursement and reduces aging balances in ways that manual follow-up processes simply cannot match.
Stage 4: Patient Account Management and The Texan Touch
Patent Applications 1407-008USU1, 1407-010USU1 (Pending)
Patient communication is not just a compliance requirement — it reflects your agency’s relationship with the community you serve. Our patient account management process, supported by pending patent-protected technology, tracks each patient account as a structured profile, analyzes interaction history and payment behavior, and dynamically adjusts payment options and communication prompts based on real-time data.
The result is what we call The Texan Touch: patients receive clear, respectful guidance and flexible payment options. Our team resolves accounts efficiently and professionally — without the aggressive or impersonal approaches that damage community trust.
Stage 5: Reporting and Analytics
End-of-Month Reports | 24/7 Client Access
Every client receives Executive and Management Summaries ready to present to their leadership team, city council, or board. You have 24/7 online access to claim status and billing performance. Transparency is not a feature — it is a standard.
What a Patented Process Means for Your Agency
When EMERGICON references a patent, it is not a marketing claim. “Our patents are a legal recognition by the U.S. government that our methods are novel, useful, and non-obvious — and no one else is doing what we do the way we do it,” said Christopher Turner, Founder, President, and CEO of EMERGICON.
For EMS leaders, that matters for three reasons:
- Defensible projections. Our patented proforma model (Patent No. 1407-003USU1) produces cash collection estimates that are documented, auditable, and grounded in real data from comparable agencies — not ballpark figures.
- Consistent outcomes. Patented processes are standardized processes. Every client benefits from the same engineered workflow, not the skill level of an individual account rep.
- Protected innovation. Our competitors cannot simply copy what we have built. The investment we have made in developing and protecting this technology is an investment in the long-term quality of your billing outcomes.
Ready to See the Difference?
EMERGICON serves more than 200 Texas EMS providers because our results speak — and now, so does our patent portfolio. If you are evaluating billing partners or want to understand what a truly engineered EMS billing process looks like, we would welcome the conversation.
To learn more, contact EMERGICON today at 866-839-3671 or support@emergicon.com.